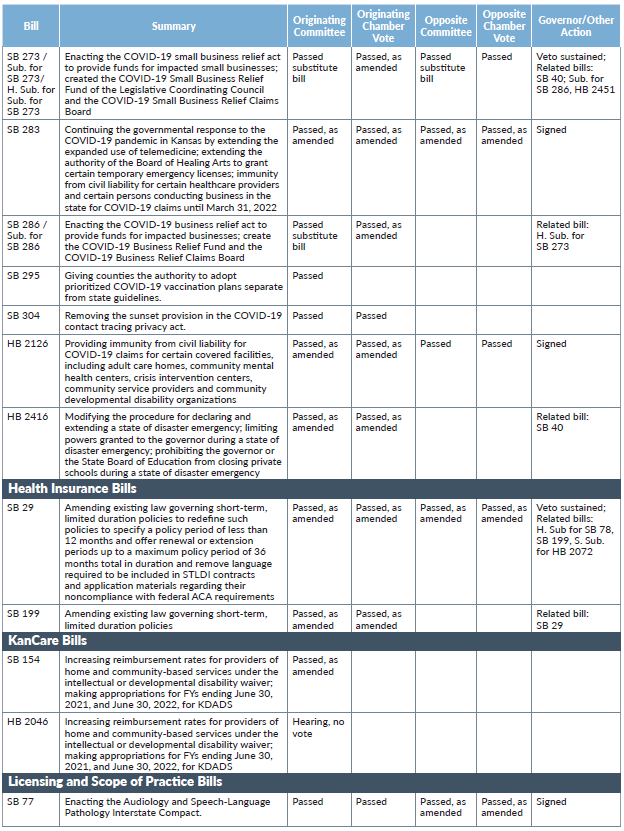
SB 283, signed by the governor on March 31, continued the governmental response to the COVID-19 pandemic by extending until March 31, 2022, (1) the expanded use of telemedicine, (2) the authority of the Board of Healing Arts to grant certain temporary emergency licenses, (3) the suspension of certain requirements related to medical care facilities and (4) immunity from civil liability for COVID-19 claims for certain health care providers and persons conducting business in the state.
HB 2126, signed by Gov. Kelly on April 9, provides immunity from civil liability for COVID-19 claims for certain covered facilities, including adult care homes, community mental health centers, crisis intervention centers, community service providers and community developmental disability organizations.
SB 273, which would have made significant changes to KEMA and the powers of the governor, the secretary of the Kansas Department of Health and Environment (KDHE), and city, county and school officials when responding to public health disasters, was significantly amended by both the Senate and House Judiciary Committees, producing two substitute bills which ultimately became H. Sub. for Sub. for SB 273 — the COVID-19 Small Business Relief Act. The final bill, which was adopted by both chambers on May 7, was vetoed by Gov. Kelly on May 21 and there was no motion to reconsider so the veto was sustained on May 26.
Sub. for SB 286 would have enacted the COVID-19 Business Relief Act to provide funds for impacted businesses; created the COVID-19 Business Relief Fund; and created the COVID-19 Business Relief Claims Board. The bill required the attorney general to administer the Act and also required certain counties and cities to establish and administer county and city COVID-19 business relief funds, respectively. The contents of H. Sub. for Sub. for SB 273 (discussed above) were replaced with the contents of this bill.
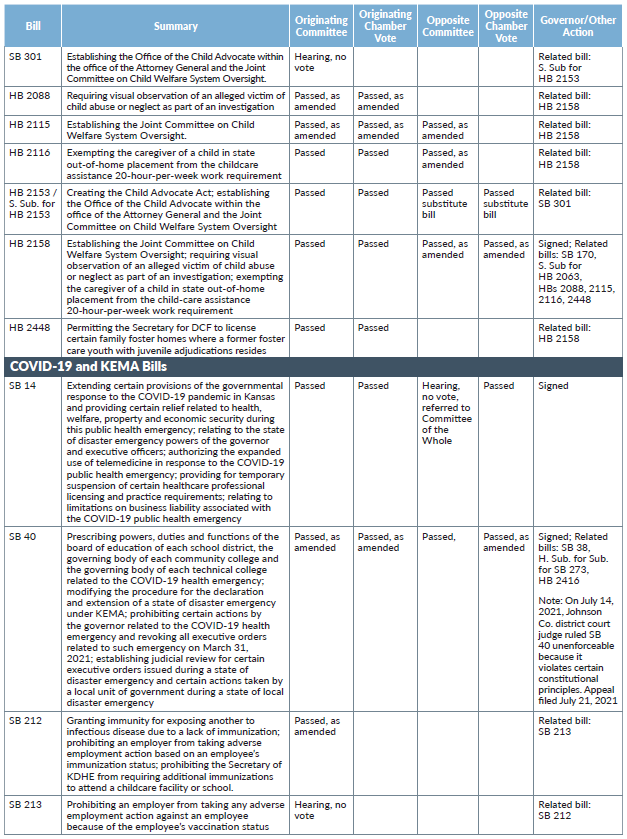
SB 212, as amended, which would have granted immunity for exposing another person to infectious disease due to a lack of immunization, prohibited an employer from taking adverse employment action based on an employee’s immunization status, and prohibited the Secretary of KDHE from requiring additional immunizations to attend a childcare facility or school, was passed favorably out of the Senate Public Health and Welfare Committee on March 29 but received no further action. SB 313, a related bill that would have prohibited an employer from taking any adverse employment action because of an employee’s vaccination status, received a hearing in the Senate Commerce Committee but no vote.
SB 159 (the Omnibus Appropriations bill) includes a proviso directing the Strengthening People and Revitalizing Kansas (SPARK) Executive Committee to be composed of three members appointed by the governor with one serving as chairperson, two appointed by the speaker of the House, and two appointed by the president of the Senate. The bill also directs that no expenditures authorized by the State Finance Council shall be made by any agency from coronavirus relief funds without prior review and recommendation by the SPARK Executive Committee for fiscal year (FY) 2022.
Behavioral Health
In January, the 2020 Special Committee on Mental Health Modernization and Reform submitted its recommendations to the 2021 Legislature. Several recommendations were discussed throughout the session, and a few key recommendations were adopted by the Legislature.
S. Sub. for HB 2208, signed by Gov. Kelly on April 22, which established rural emergency hospitals as a hospital licensure category, also established the requirements for licensure, certification and funding for certified community behavioral health centers (CCBHC), a new delivery model for behavioral health services. CCBHCs will receive cost-based reimbursement for providing a set of required services including, but not limited to, crisis services, peer and family supports, psychiatric rehabilitation services, and outpatient mental health and substance use treatment services. The Omnibus Appropriations bill, SB 159, provides $2.7 million, including $1.2 million State General Funds (SGF), for CCBHCs and 10 full-time equivalent positions for certification in FY 2022. S. Sub. for HB 2208 also (1) reduced the number of clinical supervision hours required for most masters’ level behavioral health clinicians from 4,000 to 3,000, (2) allowed clinical supervision hours to be completed via televideo, and (3) eliminated direct-client contact hours for clinical social work licensure practicums.
SB 159 also provides $3.0 million, all SGF, to support implementation and operation of the 988 Crisis Hotline. In July 2022, the National Suicide Prevention Lifeline (NSPL) will convert from a traditional 10-digit phone number to 988, similar to dialing 911 for emergency services. The 988-hotline funding will support increasing the number of calls answered by Kansas providers and help callers connect to in-state resources.
HB 2007, the base budget bill, includes $1.0 million SGF for a psychiatric residential treatment facilities pilot program in Newton for FY 2022, and up to $4 million for operation (or contract for the operation) of eight acute inpatient psychiatric beds for children in Hays or the surrounding area. For the FY ending June 30, 2022, the bill also requires the Kansas Department for Aging and Disability Services (KDADS) to expend funds to lift the moratorium on admissions to each state psychiatric hospital on or before Oct. 1, 2021 and prohibits the agency from expending funds to impose a moratorium on admissions. The same prohibition on expending funds to impose a moratorium is also included in the bill for the FY ending June 30, 2023.
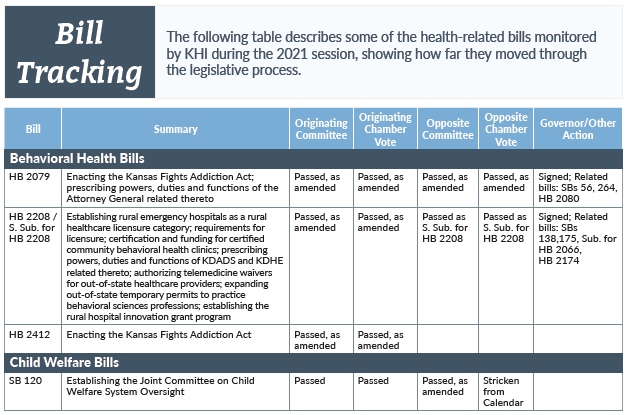
HB 2079, signed by the governor on May 21, enacted the Kansas Fights Addiction Act and established the Kansas Fights Addiction and Municipalities Fight Addiction funds. The funds will be administered by the attorney general, who is required to remit to the state treasurer all moneys received by the state from opioid litigation in which the attorney general is involved. The funds in the Kansas Fights Addiction Fund are required to be used for grants to qualified applicants for projects and activities that prevent, reduce, treat or mitigate the effects of substance use disorder and addiction.
Child Welfare
On the first day of the session, the Special Committee on Foster Care Oversight submitted its report to legislators with recommendations for program improvement and oversight. HB 2158, signed by Gov. Kelly on May 21, contained several of these recommendations, including:
-
- Establishing the Joint Committee on Child Welfare System Oversight;
- Exempting caregivers of a child in state out-of-home placement from the childcare assistance 20-hours-per-week work requirement; and
- Requiring visual observation of an alleged victim of child abuse or neglect as part of an investigation (known as Adrian’s Law).
The bill also provides certain exceptions to the confidentiality of State Child Death Review Board documents.
Licensing and Scope of Practice
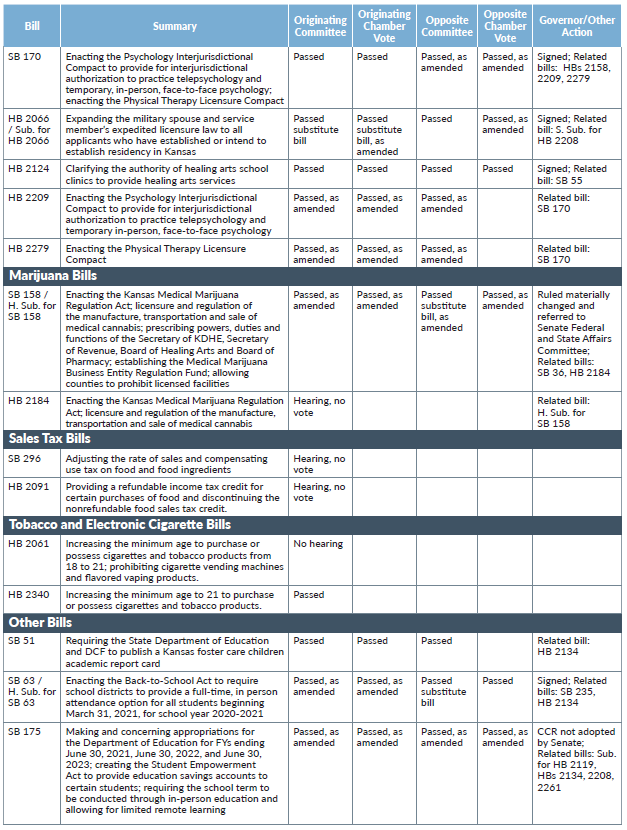
Sub. for HB 2066, signed by Gov. Kelly on April 21, shortens the period of time in which professional regulatory bodies (e.g., Board of Healing Arts, Kansas Board of Technical Professions, Behavioral Sciences Regulatory Board, Kansas Society of Certified Public Accountants) are required to issue occupational credentials to military service members or military spouses seeking to establish residence in Kansas and provides for expedited credentialing of non-military prospective residents who have received professional licensure in other states. The bill also (1) expands and clarifies existing conditions on expedited occupational credentialing, (2) permits temporary credentialing during states of emergency and the use of electronic credentials, and (3) requires licensing bodies to issue the appropriate credential to a military service member or spouse within 15 days from the date of the submission of a “complete application,” as defined by the bill, or within 45 days for all other applicants.
S. Sub. for HB 2208 enacted the Rural Emergency Hospital Act and created a category of licensure to enable certain Kansas hospitals to receive federal health care reimbursement as rural emergency hospitals (REH) and created the Rural Hospital Innovation Grant Program to provide support for eligible hospitals transitioning to the REH model.
SB 170 enacted the Psychology Interjurisdictional Compact, which allows psychologists to practice across state boundaries to offer telepsychology and allows participating psychologists to provide temporary (30 days in one calendar year) in-person psychology services. The bill also enacted the Physical Therapy Licensure Act. A third licensure compact — the Audiology and Speech-Language Pathology Interstate Compact — was enacted by SB 77.
Bills to update the scope of practice requirements for advanced practice registered nurses without a supervising physician (SB 174 and HB 2256), to expand the pharmacist’s scope of practice to include point-of-care testing for and treatment of certain health conditions (SB 200) and to provide for the licensure of dental therapists (SB 129) were once again introduced this session but failed to receive a vote following their hearings.
KanCare
Many flexibilities spurred by the COVID-19 pandemic continued for the KanCare program throughout the session, and new opportunities were included in the federal American Rescue Plan Act (ARP) of 2021, signed by President Joe Biden on March 11, 2021, including (1) 100 percent of the Federal Medical Assistance Percentage (FMAP) for COVID-19 vaccines and vaccine administration, effective April 1, 2021, through the last day of the quarter beginning one year after the COVID-19 PHE ends and (2) enhanced FMAP from April 2021 to March 2022 for Home and Community Based Services (HCBS) waivers and the Program of All-Inclusive Care for the Elderly (PACE).
Legislators also addressed reimbursement rates for some providers through the budget process. HB 2007, the base budget bill approved by the governor on April 26, continued nursing facility reimbursement rate increases of an additional $15 per day through May 1, 2021, and increased provider reimbursement rates for the Intellectual/Development Disability (I/DD) waiver by five percent for the last three months of FY 2021 and an additional two percent for FY 2022.
SB 159, the Omnibus Appropriations bill signed by the governor on May 21, extended the $15 per day nursing facility increase through June 30, 2021. Increased reimbursement rates during FY 2022 for the Technology Assisted (TA) waiver for in-home registered nurses and licensed practical nursing services were included in both HB 2007 and SB 159.
HB 2007 also requires KDADS to submit quarterly reports on the Brain Injury waiver to the Robert G. (Bob) Bethell Joint Committee on Home and Community Based Services and KanCare Oversight in FY 2022. The reports are to include the number of members enrolled in the waiver, the number of members receiving services for longer than two years and four years, and the number of members who did not receive services within a period of 60, 90 or 120 days after being enrolled.
SB 159 also raised the Protected Income Level (PIL) for FY 2022 from 150 percent of the 2019 federal Supplemental Security Income (SSI) limit (150 percent = $1,157/month) to 300 percent ($2,383/month) of the current SSI limit for HCBS waivers and PACE. Prior to changes that began two years ago, the PIL had been set at $727 per month. HB 2249, which received a hearing but no further action, would have codified the increase to 150 percent of SSI in statute.
SB 154, as amended, which would have increased reimbursement rates for providers of HCBS under the I/DD waiver and directed the Robert G. (Bob) Bethell Joint Committee on Home and Community Based Services and KanCare Oversight to study the waiting list for such services, passed favorably out of the Senate Ways and Means Committee but received no further action. The companion bill, HB 2046, received a hearing in the House Appropriations Committee but no vote.
HB 2373, which would have required KDADS to establish and implement a mobile crisis services program for individuals with intellectual and/or developmental disabilities, was passed by the House Health and Human Services Committee but received no further action.
Medicaid Expansion
On March 3, during the Senate’s deliberations on a bill related to behavioral health and telemedicine, an amendment was offered to establish the Kansas Innovative Solutions for Affordable Health Care Act, which would have expanded Medicaid, but the motion was defeated 23-12.On Jan. 12, Gov. Kelly included Medicaid expansion as a priority for the session in her State of the State message and subsequently included funding for expansion in her 2021-2022 budget proposal. For fiscal year (FY) 2022, expenditures of $596.0 million from all funds were included for expansion, with $19.0 million from the SGF. Costs for expansion also were included in her recommendation for FY 2022 caseloads. On Feb. 1, she announced a new proposal to expand eligibility for Medicaid to adults with income up to 138 percent of the federal poverty level, with components like those in 2020 SB 252, which included the creation of a new funding mechanism for the state’s share of expansion — revenue from the legalization of medical marijuana.
HB 2436, which would have enacted the Kansas Medical Marijuana Regulation Act and expanded Medicaid, and the companion bill, SB 287, were introduced in March but neither bill received a hearing and no further attempts to pass expansion were made during the remainder of the session.
If legislators choose to take another look at expansion in 2022, Congress is now providing a new financial incentive to the 12 states, including Kansas, that have not yet chosen to expand Medicaid. Under the ARP, states that do not have expansion in place are eligible for a five-percentage point increase in the state’s regular match rate, which applies to most services for children, non-expansion adults, seniors and people with disabilities, for two years if they implement expansion.
Health Insurance Regulation
A handful of bills related to health insurance received hearings during the session, but only one passed out of committee and none became law.
SB 199, introduced on Feb. 10, would have amended existing insurance law to update the term “short-term limited duration” insurance (STLDI) to specify a policy period of less than 12 months (currently 6 or 12 months) and a policy that offers renewal or extension periods of up to a maximum policy period of 36 months total in duration (currently not more than one renewal period). The bill also required the addition of a notice to consumers in STLDI contracts and application materials that these policies are not required to comply with federal Affordable Care Act requirements. Following two days of hearings in the Financial Institutions and Insurance Committee, the bill was amended to remove the notice language because similar language is already required under federal law and passed favorably out of committee. On May 6, a conference committee replaced the contents of SB 29 (related to risk-based capital instructions) with the contents of SB 199, and the bill was passed on May 7. After Gov. Kelly vetoed the bill on May 20, the House failed to override the veto on May 26.
SB 48 would have required every individual or group health insurance policy, and other types of health insurance plans that provide coverage for accident and health services and benefits for diagnostic examinations for breast cancer, to apply the same cost-sharing requirements and treatment limitations to diagnostic examinations for breast cancer that are applicable to screening examinations (i.e., mammograms) for breast cancer.
HB 2110 would have required the State Employees Health Care Commission, which administers the State Employee Health Plan, to provide coverage for the diagnosis and prescribed treatment of pediatric acute-onset neuropsychiatric syndrome (PANS) and pediatric autoimmune neuropsychiatric disorders associated with streptococcal infections (PANDAS) beginning Jan. 1, 2022. Patients, typically children, are diagnosed with PANS and PANDAS after experiencing a sudden onset of symptoms such as obsessive-compulsive disorder, tics or severe eating restriction.
HB 2157 would have required insurers, when coverage for a prescription drug or treatment is restricted by the patient’s health insurance plan through the use of a step therapy protocol, to provide patients and prescribers with a clear, readily accessible and convenient process to request an exception from the step therapy requirements.
HB 2129 would have required the State Employees Health Care Commission to provide coverage for tobacco cessation benefits for enrollees. Cessation benefits under the bill would have included any U.S. Food and Drug Administration approved medication prescribed as a tobacco cessation treatment and would have required coverage for at least four 90-day medication supported tobacco cessation attempts per year.