In response to ongoing concerns about high maternal mortality rates, some states have extended or have requested regulatory authority to extend Medicaid benefits to new mothers for up to a full year after giving birth. This A Kansas Twist blog highlights maternal health outcomes and the options that states have for extending postpartum coverage in Medicaid.
Sign up here to receive these summaries and more, and also follow KHI on Facebook, Twitter and LinkedIn. Previous editions of A Kansas Twist can be found on our ARCHIVE PAGE.
Maternal Mortality Rates
In May 2019, the federal Centers for Disease Control and Prevention (CDC), following its analysis of both national data on pregnancy mortality for 2011‒2015 and data from 13 state maternal mortality review committees (MMRC), published a report stating that “of the 700 pregnancy-related deaths that happen each year in the U.S., nearly 31 percent happen during pregnancy, 36 percent happen during delivery or the week after, and 33 percent happen one week to one year after delivery.” The CDC defines pregnancy-related death as “the death of a woman during pregnancy or within one year of the end of pregnancy from a pregnancy complication; a chain of events initiated by pregnancy; or the aggravation of an unrelated condition by the physiologic effects of pregnancy.”
The most recent report issued by the Kansas Maternal Mortality Review Committee noted that during 2016‒2018, 13 of the 57 identified deaths of women in Kansas during or within one year after pregnancy were determined to be pregnancy-related, which translates to a pregnancy-related mortality ratio (PRMR) in Kansas of 11 deaths per every 100,000 live births. The committee determined that obesity contributed to more than half of the deaths (53.8 percent) and substance use disorder contributed to nearly 1 in 4 deaths (23.1 percent).
Postpartum Coverage Under Federal Law
Under federal law, states are only required to provide 60 days of postpartum coverage for pregnant women enrolled in their Medicaid plans. However, under the federal Families First Coronavirus Response Act signed by President Trump on March 18, 2020, and amended by the Coronavirus Aid, Relief, and Economic Security (CARES) Act on March 27, 2020, states receiving enhanced federal Medicaid matching funds during the COVID-19 public health emergency (PHE), including Kansas, are required to provide continuous eligibility through the end of the month in which the PHE ends for individuals, including pregnant and postpartum women, enrolled as of March 18, 2020, or any time thereafter during the PHE, unless the person ceases to be a state resident or requests voluntary termination. The Biden administration renewed the PHE declaration on July 20, 2021, which will extend it for another 90 days, through at least mid-October, and, in a letter to state governors earlier this year, signaled that it is likely to continue the PHE through the end of 2021.
Once the PHE ends, Kansas Medicaid can, without other federal action, resume covering postpartum women for 60 days under the state plan, unless they qualify under some other aspect of the program or make less than 38 percent FPL ($10,070 for a family of four in 2021).
Extended Postpartum Coverage in Some States
In addition to the temporary extended coverage under federal law, and in response to ongoing concerns about maternal mortality rates, some states have applied for waivers to extend Medicaid benefits to new mothers for up to a full year after giving birth.
On April 12, 2021, the Centers for Medicare and Medicaid Services (CMS) approved a request by Illinois to amend its section 1115 demonstration project to enable the state to provide full Medicaid state plan benefits to postpartum women with income up to 208 percent of the federal poverty level (FPL) for 12 months, inclusive of the 60-day postpartum period under its state plan. Georgia also has received CMS approval for its demonstration project, which will test the effects of extending to six months full Medicaid state plan benefits to postpartum women with income up to 220 percent (after 5 percent income disregard) FPL. In Missouri, a recently approved demonstration project will test the effects of providing “robust” behavioral health benefits — including substance use disorder (SUD), mental health and non-emergency medical transportation services — for an additional 10 months following the end of the 60-day postpartum period to certain postpartum women who have been diagnosed with an SUD and who have income up to 196 percent (after 5 percent income disregard) FPL.
In February 2020, New Jersey submitted an application to CMS seeking to extend coverage to 180 days postpartum, but only for women who meet all other requirements for the state plan and who have family income greater than 138 percent FPL and, thus, do not qualify for continued coverage through the Affordable Care Act’s Medicaid expansion provisions. The state is still waiting for approval of this application. Virginia’s application, submitted on March 31, 2021, seeks to provide coverage for 12 months postpartum for pregnant women with income below 205 percent FPL who are currently not eligible to transition to another coverage group postpartum.
Additional states are already considering taking action in the future to provide extended coverage to pregnant women under federal law signed by President Biden earlier this year. A provision in the federal American Rescue Plan Act of 2021 (ARP), effective on April 1, 2022, gives states the opportunity, for five years, to extend Medicaid and Children’s Health Insurance Program eligibility to pregnant women for 12 months postpartum. States choosing this option would be required to provide full Medicaid benefits for women during the 12 months following pregnancy.
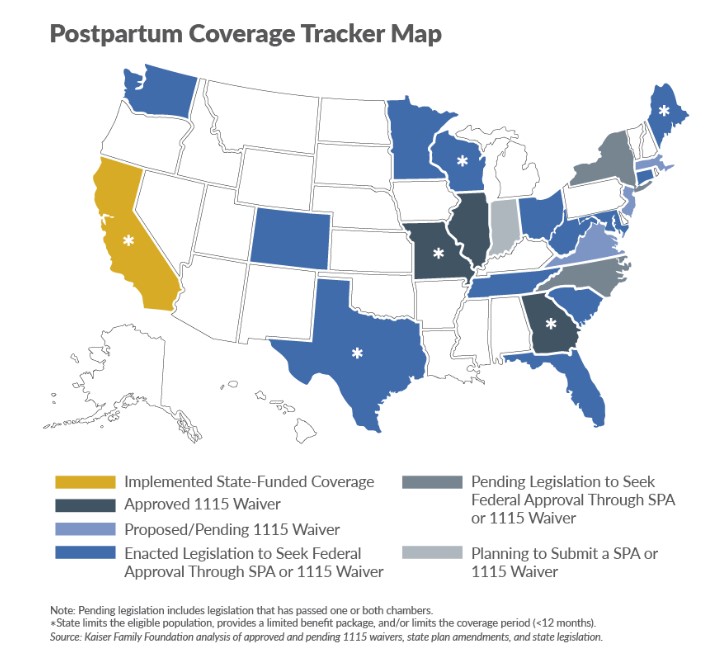
On June 3, 2021, Indiana withdrew from CMS a section 1115 demonstration application submitted last year that sought authority to extend Medicaid coverage from 60 days to 365 days for postpartum mothers who (1) have an opioid use disorder, (2) initially qualified for Medicaid with income at or below 213 percent FPL, (3) maintain continuous eligibility for themselves and their babies during the entire postpartum period; and (4) participate in Indiana’s Maternal Opioid Misuse cooperative agreement, which was awarded to the state by the CMS Center for Medicare and Medicaid Innovation in December 2019. However, the state noted in its withdrawal letter to CMS that it intends to pursue the broader postpartum coverage provided for under the ARP. Massachusetts submitted a section 1115 application on June 8, 2021, seeking authority to implement continuous postpartum coverage consistent with the option in the ARP but asked that it be effective prior to the April 1, 2022, effective date in the federal law and without regard to immigration status. At least a dozen other states have enacted legislation, have pending legislation or are planning to seek federal approval for coverage extensions either through state plan amendments or a section 1115 waiver (see map).
Gov. Laura Kelly’s Commission on Racial Equity and Justice recently released its July 2021 report which includes a recommendation to extend Medicaid coverage for mothers through 12 months.