In their complaint, the plaintiffs asked the court to declare the work requirements policy and Kentucky’s waiver illegal so it cannot be implemented. They assert that HHS “bypassed the legislative process and acted unilaterally to ‘comprehensively transform’ Medicaid” and put them at risk of losing their coverage by creating new eligibility criteria. In its policy guidance issued in January, CMS stated that it was allowing work or community engagement waivers to test whether they will result in more beneficiaries being employed or engaging in other community activities that would produce improved health and well-being. In issuing the work requirements guidance and approving Kentucky’s waiver, HHS relied on its authority under Section 1115 of the Social Security Act, which permits HHS to waive certain provisions of federal Medicaid law to allow states to undertake demonstration projects that the Secretary determines will further program objectives.
In a memorandum filed with the court on April 25, 2018, the federal government argued that Section 1115 gives the secretary broad authority to approve state demonstration projects and that it complied with all required Administrative Procedure Act standards. The government also characterized Kentucky’s program as an experimental project designed to “test innovative methods to promote health” for members of its Medicaid expansion population.
On June 29, 2018, Judge James E. Boasberg issued an opinion in the case and vacated Secretary Azar’s approval of Kentucky’s work requirements program. In his opinion, Judge Boasberg stated that while the secretary has broad discretion to approve demonstration projects like Kentucky’s, he found that the secretary had not adequately considered whether the project would, in fact, further the objectives of the Medicaid program and help the state furnish medical assistance to its citizens. He also stated that his review of the administrative record showed the secretary had not “adequately considered” how many people might lose coverage if the waiver was approved. In vacating the waiver, the court remanded, or returned, the waiver to HHS to correct the error and issue a decision supported by the administrative record. In the meantime, the court’s decision prevents Kentucky from implementing its work requirements program.
HHS and Kentucky have 60 days to appeal Judge Boasberg’s decision and CMS officials have indicated they are conferring with the U.S. Department of Justice about how to proceed. Although the court’s decision only impacts Kentucky’s waiver, states with pending waiver applications will certainly be watching to see how the case is resolved.
The ‘Subsidy Cliff’
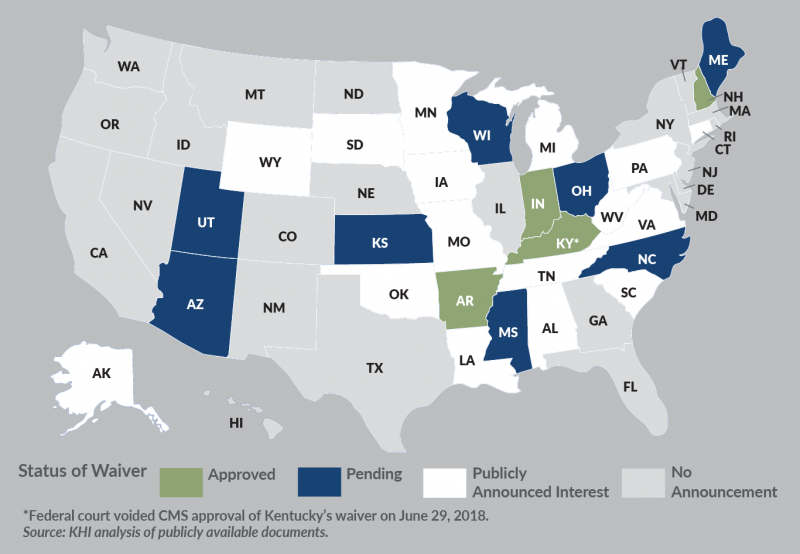
On May 1, 2018, CMS Administrator Seema Verma expressed concerns about individuals who might lose coverage if CMS were to approve work requirements in states such as Kansas that have not expanded Medicaid. She referred to the “subsidy cliff” that would occur if individuals begin to earn enough income to make them ineligible for Medicaid but not enough to qualify for financial assistance (tax credits) on the Affordable Care Act (ACA) marketplaces. In addition to Kansas, the non-expansion states of Maine, Mississippi, North Carolina, Utah and Wisconsin have also submitted proposals for work requirements as a condition of eligibility for their Medicaid programs. While Ms. Verma did not rule out approving work requirement waivers for non-expansion states, she stated that CMS was seeking solutions to address the subsidy cliff.
On May 23, 2018, South Dakota, a non-expansion state, posted a draft proposal on its website to implement a pilot Medicaid work requirements program, entitled the Career Connector program, in two of its most populated counties. However, it appears the state is attempting to address CMS’s concerns about the subsidy cliff by providing “Transitional Medical Benefits” for a period of 12 months to individuals who lose eligibility due to increased earnings. As enrollees make more money, the state would move them into a premium assistance program to help them purchase employment-based insurance or coverage through the ACA marketplace. The program would provide these individuals with coverage assistance until they reach 150 percent of FPL for one year when they would be eligible for both premium tax credits and cost-sharing subsidies for marketplace coverage. The proposal indicates that the state will finance the non-federal share of expenditures using state general funds.
KanCare 2.0
In the KanCare 2.0 renewal application submitted to CMS on December 26, 2017, the state proposed the implementation of work requirements for “some able-bodied” adults on or after January 1, 2019. Unlike the states whose work requirements have already been approved, Kansas has not expanded Medicaid and is proposing to apply its work requirements to some of its otherwise-eligible adults. KanCare members who would not be subject to the work requirements include:
-
- Members receiving long-term care, including institutional care and Money Follows the Person;
- Members enrolled in or on the waiting list for Home- and Community-Based Services waiver programs;
- Children (age 0-18);
- Pregnant women;
- Members who have disabilities and are receiving Supplemental Security Income (SSI);
- Caretakers for dependent children under 6 years or those caring for a household member who has a disability;
- Medicaid beneficiaries who have an eligibility period that is only retroactive;
- Members enrolled in the MediKan program;
- Members presumptively eligible for Medicaid;
- Persons whose only coverage is under a Medicare Savings Program;
- Persons enrolled in Programs of All-Inclusive Care for the Elderly (PACE);
- Members with tuberculosis, HIV or in the Breast and Cervical Cancer Program;
- Members who are age 65 years and older; and,
- Certain caretakers of KanCare members age 65 and older who meet criteria specified by the state.
The state proposes to assess beneficiaries at the point of application or redetermination to determine if they would be required to meet the work requirements. Similar to the requirements already in place for its existing Temporary Assistance for Needy Families (TANF) program, the minimum weekly work requirement would be 30 hours in a one-adult household without children under age 6. Under TANF, the requirement for one-adult households with a child under age 6 is reduced to 20 hours; whereas under KanCare 2.0 the work requirement would be eliminated entirely. Minimum weekly requirements in two-adult households would be 35 hours for households not using subsidized childcare and 55 hours for those that do. For any given individual, the maximum requirement is 40 hours per week.
Activities that would meet the state’s definition of work include:
-
- Unsubsidized employment, full or part-time;
- Subsidized public employment, such as temporary staffing, federal work study, Job Corps, or Workforce Innovation and Opportunity Act paid work experience in which wages are subsidized by TANF or other public funds;
- Subsidized private employment in which wages are subsidized by TANF or other public funds;
- Work experience, such as an unpaid, supervised assignment to help the member develop work history, improve work habits and increase self-confidence and esteem;
- On-the-job training;
- Supervised community service;
- Vocational education;
- Job search/job readiness activities;
- Job readiness case management (one-on-one services);
- Job skills training directly related to employment;
- Education related to employment, including adult basic education, English as a Second Language, and other courses designed to provide knowledge and skills for a specific job; and,
- Secondary school attendance, including efforts toward GED or completing a high school degree.
Members who fail to comply with the work requirements would be removed from KanCare until compliance is achieved. Disenrollment would occur the first day of the month following the month in which the member was found to no longer meet the work requirements. The disqualification period would continue until the member complies with all work requirements.
The current KanCare program provides for transitional Medicaid coverage, referred to as TransMed, which is designed to provide temporary health coverage to families moving to economic self-sufficiency. Similar to the South Dakota proposal, TransMed provides an additional 12 months of coverage for families who were previously eligible for Medicaid but who lost eligibility due to increased earnings. In the KanCare 2.0 renewal application, the state said it is considering the creation and funding of “Independence Accounts,” a type of health savings account, for adults enrolled in TransMed, to encourage them to maintain employment and transition out of Medicaid into private coverage. Unlike South Dakota’s proposal, the Kansas TransMed program description does not indicate that transitional assistance would remain in place until enrollees reach at least 150 percent of FPL.
Kansas Work Requirements Survey
In late 2017, Commonwealth Fund and REACH Healthcare Foundation commissioned researchers from the Harvard T. H. Chan School of Public Health at Harvard University to conduct a telephone survey of Kansans, ages 19-64, and with family incomes at or below 138 percent of the federal poverty level (who would presumably be eligible if the state expanded Medicaid). When asked about the implementation of work requirements in the Kansas Medicaid program, of those currently enrolled in Medicaid or without any insurance coverage, 49 percent reported that they were already working, 34 percent had a disability that kept them from working, and only 17 percent were otherwise not working. Breaking down the 17 percent who were otherwise not working, 11 percent said they would be more likely to look for work if that was required to obtain Medicaid, and 6 percent said they would not be more likely to look for work even if required.
Opposition to Work Requirements
In addition to the lawsuit filed by Kentucky Medicaid enrollees, numerous national groups and organizations representing health care, disability rights, criminal justice and faith-based organizations have expressed their opposition to work requirements. On February 15, 2018, 160 organizations— including the National Alliance on Mental Illness (NAMI), the Center for Law and Social Policy (CLASP), the American Heart Association/American Stroke Association, the American Lung Association and the American Diabetes Association—sent a letter to HHS Secretary Alex Azar expressing their concerns about the CMS decision to approve work requirements in Medicaid. The most commonly cited concerns included:
Some individuals who do not meet the Social Security disability requirements may have a chronic illness or disability that would prevent them from gaining or retaining employment;
Some individuals with criminal records may not be able to secure employment or even engage in volunteer activities;
Work requirement programs will require significant state investment in infrastructure, will necessitate new administrative processes and programs, and will require considerable financial and human resources;
The effectiveness of work requirements implemented in other social service programs—such as SNAP, TANF and federal housing programs—have not consistently produced an increase in stable employment or financial independence;
Individuals who are no longer eligible for Medicaid will likely wait to seek care until their conditions are more serious and costly to treat; and,
Work requirements could lead to higher uninsured rates and an increase in emergency room visits.
Conclusion
With the Trump administration’s support of Medicaid work requirements, it is likely that the states that have already submitted, or plan to submit, Section 1115 demonstration proposals will soon receive approval for those programs. However, non-expansion states may be asked to modify their proposals to include additional program elements addressing CMS concerns about the “subsidy cliff.” This may prove challenging if these alternative coverage provisions require states to fund additional costs.