Introduction
The U.S. Department of Health and Human Services (HHS) released final summary enrollment data on April 3, 2018, for the fifth open enrollment period of the federally facilitated health insurance marketplace created by the Affordable Care Act (ACA). The open enrollment period for the 2018 plan year lasted only 45 days, from November 1, 2017, through December 15, 2017 (with a run-out period until December 23, 2017), for individuals who wished to purchase individual health insurance through the marketplace for coverage beginning on January 1, 2018. The open enrollment periods for the 2016 and 2017 plan years were three months long, from November 1 through January 31. The ACA still allows some consumers to enroll for 2018 marketplace coverage outside of the open enrollment period if they experience a “life event” (e.g., loss of previous coverage or change in family status) and enroll within 60 days from the date of that qualifying event.
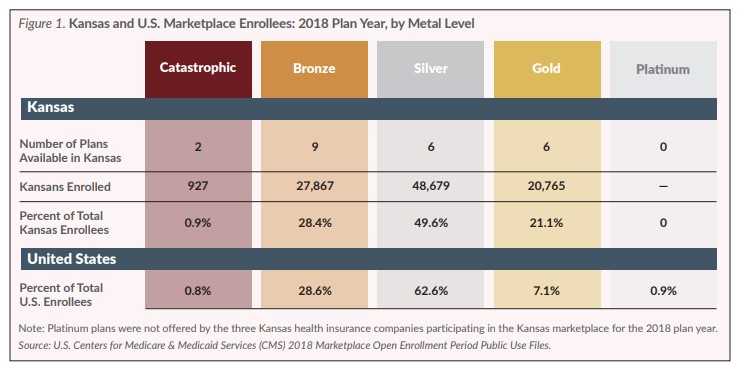
For 2018 open enrollment, three insurers offered coverage on the marketplace in Kansas. Medica Insurance Company offered plans in every county in the state. Sunflower Health Plan entered the marketplace for the first time and offered plans only in Johnson and Wyandotte counties. Blue Cross and Blue Shield of Kansas offered plans in all counties except Johnson and Wyandotte.
This brief looks back at the results of this fifth open enrollment period, which was for plan year 2018, during which 98,238 Kansans and 11.8 million consumers nationwide selected or were automatically re-enrolled in a marketplace plan. Despite the uncertainty regarding the future of the ACA, including the individual mandate, enrollment in the Kansas marketplace was essentially unchanged in 2018 (542 fewer Kansas enrollees) and 3.8 percent lower nationally (465,828 fewer enrollees).
Enrollee Characteristics
The data from HHS show that 121,151 Kansans shopped for a marketplace plan for 2018 and were determined eligible to enroll, but only 98,238 Kansans completed their enrollment and selected a plan or were automatically re-enrolled. Nearly three-quarters (72.2 percent or 70,905) of Kansans selecting a marketplace plan had been enrolled in 2017. There were 52,465 active re-enrollees, of which half (50.3 percent or 26,404) switched plans. Another 18,440 returning enrollees were automatically re-enrolled by the marketplace. More than one-quarter (27.8 percent or 27,333) of Kansas enrollees were “new consumers” who did not have marketplace coverage in 2017. HHS has not yet released information on the percentage of enrollees who have “effectuated” their enrollment by paying their premiums.