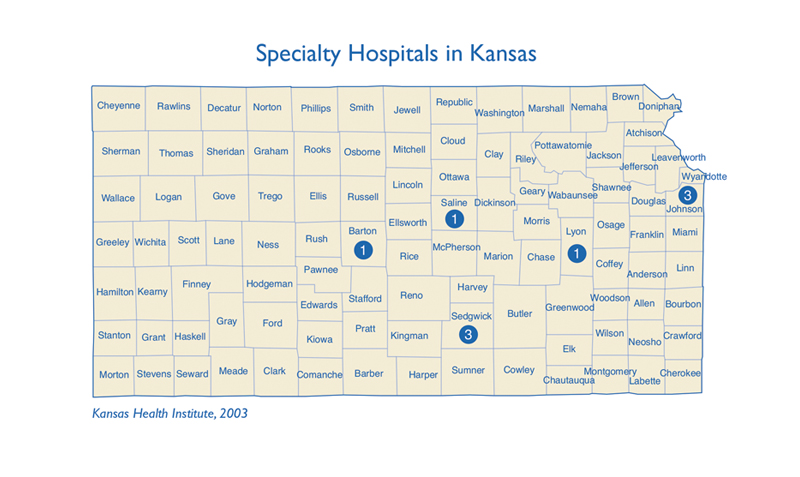
High payments exist in part because Medicare, the federal health insurance program for the aged and disabled and the predominant payer for these types of procedures, may not be adjusting for changes in technology which have lowered the costs of services. Although general hospitals are also likely to be earning profits on these services, they have used these profits to cover the costs of unprofitable health care services that benefit the community, such as 24-hour emergency room care, intensive care units, and care for the uninsured.
Specialization and Quality
Specialty hospitals claim to offer high quality through newer facilities, better equipment, and specialization. To be sure, some patients will favor a new specialty hospital’s amenities and location but claims of higher quality care have not yet been validated. New specialty hospitals may have an opportunity to provide newer technologies than existing hospitals. However, newer technology does not always lead to an improvement in quality, and general hospitals can adopt these technologies as well.
Specialty hospitals also claim higher quality because of the notion that “practice makes perfect.” Research confirms that experienced teams who frequently repeat procedures become more proficient, but both general and specialty hospitals can benefit from high volumes of procedures. It is unclear whether specialty hospitals’ narrow focus on a specific set of procedures will lead to higher patient volume for these procedures as compared to a community’s general hospitals. Moreover, even if higher volume did lead to better quality at a particular specialty hospital, the average quality of care in that community might decline if the newer hospital drew away cases that the specialist teams in general hospitals needed to maintain their skills.
Physician-owners of specialty hospitals have a financial incentive to refer patients whose conditions are less severe (which critics call “cream-skimming”) to their hospitals. Because healthier patients are less expensive to treat and are more likely to have good outcomes, specialty hospitals can benefit from this selective referral both financially and in quality comparisons. The U.S. General Accounting Office found evidence that specialty hospitals benefit from selective referral, which casts doubt on the quality claims made by specialty hospitals and leaves the impression that there is an uneven playing field in the market for specialty patients.
Impact on Community Health Services
The threat posed by specialty hospitals to general hospital profitability is real, but is it a matter for public policy concern? The answer depends on the perceived value of the community services provided by general hospitals. General hospitals not only provide their communities with unprofitable health care services, but also community Specialty Hospitals in Kansas health services like disease prevention screenings and health education. Many non-profit general hospitals care for the poor and underserved in fulfillment of their mission. For-profit general hospitals may also provide a certain level of charity care. General hospitals may benefit from the goodwill generated by providing such services, but the cost of providing them is implicitly subsidized by the margins earned on profitable health care services. The growth of specialty hospitals threatens the use of these implicit subsidies to fund community health services.
In the communities where they exist, specialty hospitals already threaten these subsidies, but we do not yet know whether community services have been affected. The threat to general hospitals could lead some of them to develop strategies to compete with or pre-empt specialty hospitals. For example, they could change the way they operate surgical units, upgrade facilities or partner with physicians to build their own specialty hospitals. Their alternative is to try to scale back or find other sources of funding for the community services they provide. In communities where the threat has yet to emerge, policymakers may wish to maintain the system of subsidizing unprofitable services with overall profit margins within full-service hospitals. Maintaining this traditional method of financing community health services may require that policymakers raise barriers for specialty hospitals to make it more difficult for them to compete.
Policy Options
There are a number of responses to the emergence of specialty hospitals that policymakers could consider:
-
- Wait and see.
Before taking any action, policymakers may want better information about the financial status and quality of care at general hospitals and specialty hospitals. These data may not be available for some time and could require additional reporting by hospitals of both types. In the meantime, federal reform of Medicare payments might reduce the relative profitability of specialty hospitals. If Congress does not step in, though, more specialty hospitals could be built.
- Remove the conflict of interest for physician-owners of hospitals.
Another option for policymakers is to level the competitive playing field by removing the incentive physician-owners have to divert patients towards specialty hospitals. Medicare forbids physicians from referring patients to health care facilities in which they hold a direct investment, under provisions of federal law attributed to Representative Pete Stark (D-CA). However, the ban does not apply to physicians who have invested in hospitals. The Medicare reform and prescription drug bill recently passed by Congress temporarily extends the ban on physician self-referrals to new specialty hospitals (See box on page 2). Nevertheless, states could decide for themselves to make such a moratorium permanent and whether or not to extend the moratorium to existing facilities. Legislatures in Ohio, Illinois, New Mexico, and Washington, among others, have introduced legislation that would prohibit physician investment in specialty hospitals.
- Require specialty hospitals to expand services.
Requiring specialty hospitals to provide broader emergency services or to meet some specified level of community or charity care would spread the costs for these services but could also weaken any advantages that stem from specialty hospitals’ narrow focus. The initial financial success of specialty hospitals has raised the question of whether it is more efficient for health care facilities to specialize or to provide centralized delivery of a wide range of health care services. Requiring specialty hospitals to broaden their mission could make it more difficult to answer this question.
- Re-establish certificate of need requirements.
Another option for preserving critical community health care services is to reinstate a Certificate of Need (CON) process to regulate construction of new specialty hospitals. Kansas, among other states, eliminated CON in 1985 in favor of a market-oriented approach to the allocation of health care investments, patients, and profits. States that retained CON, such as Missouri, have a regulatory tool to limit the spread of specialty hospitals, and very few specialty hospitals have been built in those states. However, it may be difficult to limit the scope of CON to the specialty hospital issue, just as it may be difficult to insulate the CON process from undue political influence.
- Provide direct financing for community health services.
Implicit subsidies within general hospitals are not the only way to finance community health services. Alternatives include increasing direct subsidies to hospitals for treating large numbers of poor and uninsured patients. Other options for ensuring access to critical health care services include expanding health insurance coverage and providing additional funding to local health departments for health care and community health services.