Several Barriers Affect Identification, Referral
Kansas physicians reported multiple barriers to identifying, referring and treating mental health conditions in young children. Most commonly these barriers related to referrals, such as long wait times or a lack of qualified providers. Physicians also cited barriers related to their own competence, and these were most likely to influence their identification, referral and treatment practices. Examples included lack of training or lack of confidence in their ability to identify or treat young children with mental health conditions.
How Barriers Relate to Inquiry, Referral and Treatment
Survey results showed relationships between how Kansas physicians rated barriers and what they reported about identifying, referring and treating mental health conditions in young children.
-
- Physicians who reported greater concerns about their ability to diagnose and treat mental health conditions were less likely to inquire about or treat children with mental health conditions. But they were more likely to refer children to mental health services.
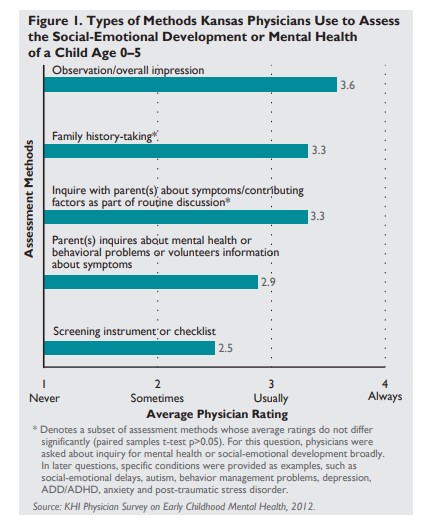
- Physicians who used screening instruments tended to report inquiring more frequently about a range of specific mental health conditions. Physicians who reported using more informal assessment methods were more likely to report referring children to services.
-
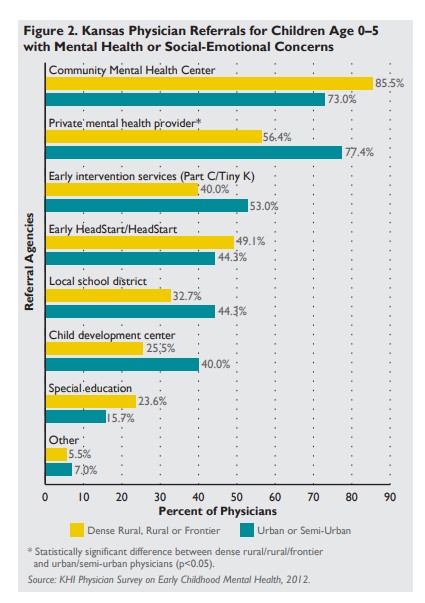
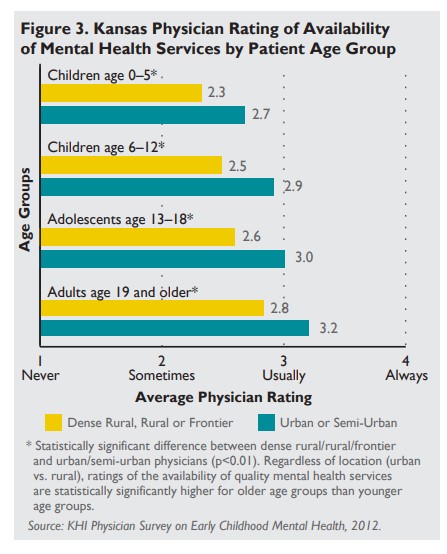
- Physicians who gave higher ratings for availability of quality mental health services for children age 0–5 were more likely to report referring children and did so more frequently.
- Physicians who practiced in urban settings were somewhat more likely to report inquiring about specific mental health conditions.
- Physicians in solo practice were somewhat less likely to report inquiring about specific mental health conditions than those in group or other practice settings.
What Does This Mean for Mental Health Policy in Kansas?
Because early intervention for Kansas children with mental health conditions could minimize future problems and prevent more intensive service needs in the future, state policymakers and providers should consider ways to enhance screening, referral and connection to services for young children.
-
- Educate physicians about screening young children for mental health conditions.
Physicians who reported concerns about their abilities to diagnose and treat mental health conditions were less likely to inquire and treat young children. Many physicians also reported interest in further education about identifying mental health concerns in young children. These results point to the need for additional education for primary care physicians about screening. Existing efforts by KAAP and KAFP to educate members about screening practices in primary care should be continued and expanded if possible, to target specific groups of physicians who are less likely to screen, such as those in solo practice or rural settings.
State agencies like the Kansas Department of Health and Environment or the Kansas Department for Aging and Disability Services also could build on existing efforts by offering complementary training for physicians on screening young children, as is done in at least 17 other states.
-
- Ensure availability of quality mental health services for young children, particularly in rural communities, and encourage cross-system coordination and connection to services.
Kansas physicians who reported that quality mental health services were available for children age 0–5 were somewhat more likely to refer children to services. In order to improve identification and referrals through screening, and ultimately to improve access to these services, quality services should be consistently available on a statewide basis.
Continuing and expanding efforts to provide professional development and early childhood mental health accreditation, or endorsement, for providers may help increase the workforce capacity. Because rural physicians were less likely to say that quality services were available, it is particularly important to explore models to better recruit and retain early childhood mental health providers in rural areas. In addition, connecting physicians with early childhood and mental health resources in their communities may increase awareness of existing services.
With movement toward care coordination and medical home models in the proposed Medicaid reform (KanCare), Kansas policymakers may have an opportunity to integrate more mental health screening into the primary care medical home structure. Having mental health professionals work in offices with physicians has been shown to increase the availability of services and effectively address young children’s social-emotional development within their medical homes.