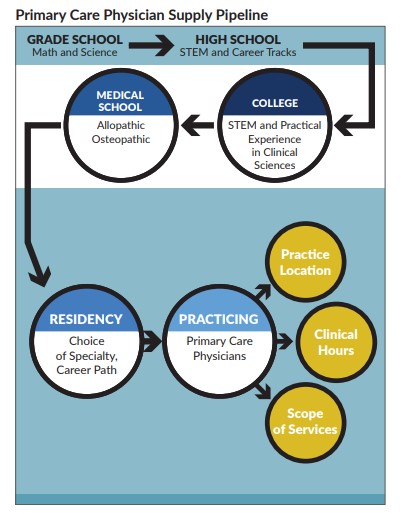
Strategies to Address the Workforce Shortage
The state should consider collaborative and innovative approaches to efficiently deliver primary care services and address regional disparities. A combination of efforts to train more primary care physicians in Kansas, recruit more to the state and retain current physicians will be necessary.
Training
To increase the number of PCPs practicing in Kansas, one strategy could be to increase the number of medical school and residency positions in the state which have not kept pace with increases nationally. Recent developments hold promise for increasing the number of PCPs in Kansas:
-
- The bipartisan Resident Physician Shortage Reduction Act of 2019 (S. 348, H.R. 1763) was introduced to increase the number of medical resident training positions by 15,000 over the next five years. A provision of the bill states that at least 50 percent of the new residency slots are to be used for a shortage specialty residency program.
- The Community Health Center of Southeast Kansas (CHC/SEK) received a $750,000 grant from the Health Resources and Services Administration (HRSA) for its new Rural Residency Planning and Development Program (RRPD) in Family Medicine, a collaboration with the University of Kansas School of Medicine. The residency program will initially train two physicians annually, with a plan to eventually graduate four physicians from the program each year.
- Increasing the number of medical students trained in Kansas either at the KU campuses or through the proposed new osteopathic medical school in Wichita.
Recruiting
Training strategies could be coupled with recruitment strategies to bring more PCPs to the state and to encourage students to pursue a career in medicine and primary care. For example, some programs target high school students to encourage them to consider health professions as a potential career, particularly in rural areas. Another option to strengthen the primary care workforce includes recruiting medical professionals via federal and state loan repayment programs.
The National Health Services Corps (NHSC) helps repay qualified loans in exchange for a two-year commitment to provide health care services in eligible Health Professional Shortage Areas (HPSA). There were 84 Kansas participants — including physicians, dentists and other clinicians — in the NHSC program in 2018. The State Loan Repayment Program (SLRP) offers similar assistance, and from 2011 to 2018 there were 13 physician awardees of the SLRP in Kansas. While more provider specialties have been made eligible for the SLRP, federal funding was reduced from $150,000 to $135,000 in 2018, while state funding remained the same at $150,000.
The Kansas Medical Student Loan Program (MSLP) offers full tuition payment and a $2,000 monthly stipend for up to 30 students each year (120 at any given time) in return for agreements to practice primary care in underserved areas in Kansas. Under the Kansas Bridging Plan (KBP), the state funds up to 13 PCP slots annually in exchange for a three-year commitment to practice in rural communities. Since 1991, 337 residents have enrolled in KBP, and of the 245 physicians that have completed the program, 85 percent continue to practice in Kansas. Finding new funding sources or increasing state funds for loan repayment programs might improve recruitment of PCPs.
Kansas also has recruited international medical graduates, physicians who earned their degrees in another country. Kansas participates in the J-1 Visa Exchange Visitor Program, which allows up to 30 international medical graduates to practice medicine full-time for a minimum of three years in a federally designated HPSA in Kansas.
Retaining
Retaining physicians is an important way to reduce workforce shortages. Ways to retain physicians might include lowering the cost of medical malpractice insurance, allowing flexible work schedules or finding other ways to address provider wellness. While few promising strategies have yet emerged to address provider wellness, one strategy could be collaborative team-based practice. Research suggests PCPs could increase the number of patients they can serve — referred to as panel size — using health care teams comprised of clinical (i.e., physician assistants and nurse practitioners) and nonclinical staff, who offer a broad set of skills which complement and improve the efficiency of PCPs. The PCP could achieve a reasonable panel size through effective team-based task delegation and potentially avoid burnout or other stressors. Recent federal policies are designed to reward value and care coordination, reinforcing the need for a reasonable panel size to ensure high-quality outcomes.
In addition, some states, such as Alabama, offer tax credits to encourage PCPs to practice in a federally designated HPSA. Finally, adopting and streamlining new technological innovations under telemedicine or telehealth tools could increase access to care and reduce administrative burden.
Conclusion
While the need to expand the PCP workforce is heightened by both an aging workforce and an aging population, innovative approaches could help better prepare the state for future needs, especially in rural areas. Further, more consistent collection and analysis of critical information by licensing authorities is needed to effectively understand, manage and build the PCP workforce.