The ACA and Mental Health Coverage
Provisions within the Affordable Care Act (ACA) may result in an increase in insurance coverage, particularly for people with mental illness. These individuals will no longer be denied coverage due to pre-existing mental health conditions, nor can they be charged higher rates for coverage. Existing federal and Kansas mental health parity laws and new federal requirements within the ACA have enhanced the coverage of mental health services in private insurance plans in recent years, requiring that coverage be equivalent to the coverage provided for physical health services. In addition, the ACA created marketplaces for individuals to purchase private insurance using federal tax credits if they qualify.
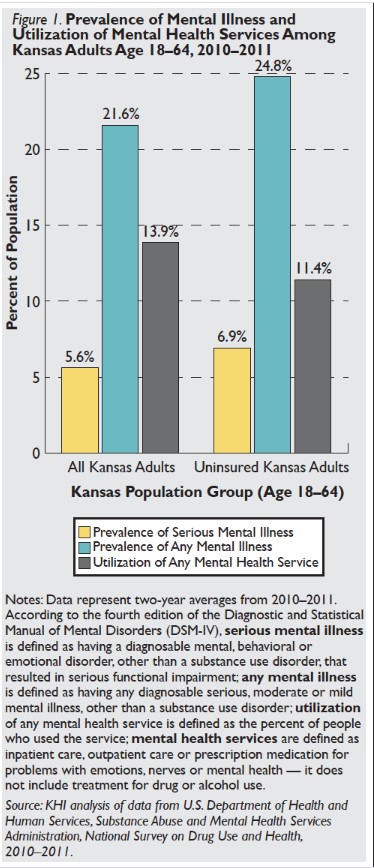
Estimates from SAMHSA indicate that increasing insurance coverage through the ACA will increase utilization of mental health services. About 186,000 uninsured Kansans with incomes between 100 percent and 399 percent of the federal poverty level (FPL) are likely eligible for tax credits to purchase private insurance through the federal marketplace. In 2011, 16.5 percent of these uninsured Kansans who are likely eligible for tax credits utilized some type of mental health service, including medication. SAMHSA estimates that utilization of mental health services may increase by as much as 25 percent when this group gains insurance coverage. If everyone who was uninsured and eligible for tax credits through the marketplace gained insurance, the mental health system could realize an additional 7,700 patients.
States have the option under the ACA to expand Medicaid eligibility to adults up to 138 percent of FPL, which is about $32,900 annual income for a family of four. The state of Kansas has decided not to expand Medicaid. The utilization rate for uninsured Kansas adults with incomes at 138 percent of FPL or less was 10.5 percent, and SAMHSA estimates that this utilization rate would increase to 14 percent if Medicaid was expanded. Even without expansion, Kansas will likely see an increase in enrollment and mental health service utilization as some adults currently eligible for, but not enrolled in, Medicaid decide to enroll due to the individual mandate of the ACA and increased publicity about the law. This enrollment increase is known as the “welcome mat” or “woodwork” effect.
Provider Shortage
With the expectation that more patients will enter the mental health system, questions must be raised about the supply of mental health providers in local communities to meet this increased demand.
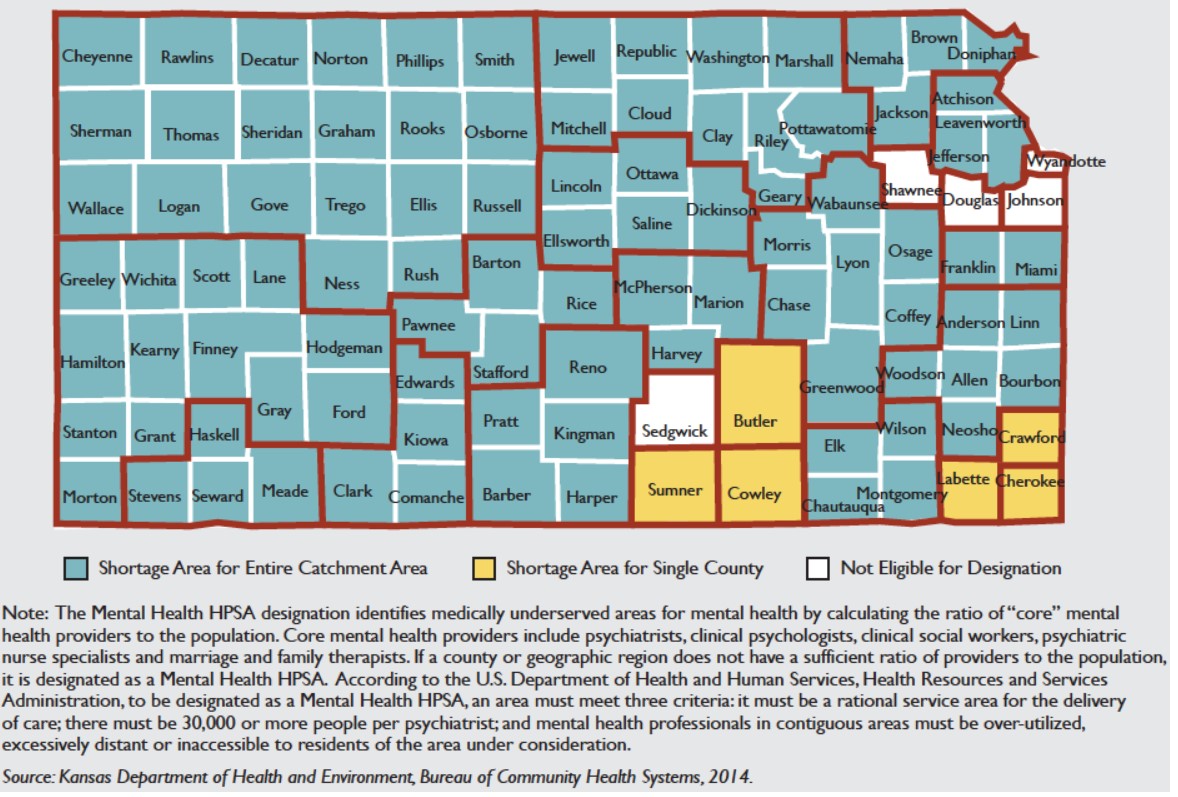
As shown in Figure 2, nearly all Kansas counties (100 out of 105) have been designated by the federal government as Mental Health – Health Professional Shortage Areas (HPSAs). This means that the ratio of mental health providers to the population is not sufficient according to the criteria established by the federal government. All Kansas counties except Douglas, Johnson, Sedgwick, Shawnee and Wyandotte have been identified as Mental Health HPSAs. There are some parts of those counties that also have the designation. Approximately 47 percent of Kansans live in a county that is, in its entirety, a Mental Health HPSA.