Other Adults in Medicaid
There are other adults eligible for Medicaid in addition to those already described. These adults make up less than 1 percent of all Medicaid or CHIP beneficiaries. These adults are covered due to severe health conditions such as tuberculosis, AIDS and breast or cervical cancer. The ACA requires that young adults who are in foster care and are covered by Medicaid when they turn 18 remain eligible until age 26. In addition, children in the juvenile justice system are automatically eligible for Medicaid coverage until they turn 21.
Costs of Adults in Medicaid
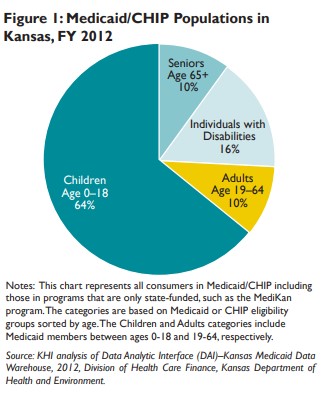
Health care costs for non-elderly, non-disabled Kansas adults in Medicaid totaled $248 million in fiscal year 2012, accounting for 9 percent of the total $2.8 billion spent on Kansas Medicaid and CHIP that year. Based on administrative data from the Kansas Department of Health and Environment (KDHE), health care spending for these adults in Medicaid averages about $6,500 annually per enrollee. This is about half of the cost of an elderly person in Medicaid and one-third the cost of a person with disabilities in Medicaid. Compared with other Medicaid adults, the elderly and adults with disabilities tend to use more expensive care, such as nursing facilities and other long-term care services and support.
Spending for non-disabled adults under age 65 is about three times the cost of a child in Medicaid or CHIP, on average. Much of the cost difference between children and adults can be attributed to the costs for prenatal care and labor and delivery coverage for pregnant women in this population.
As of January 1, 2013, Kansans eligible for Medicaid receive care through one of the three managed care organizations (MCOs), collectively organized under KanCare. These MCOs coordinate primary care, physical and behavioral health care, community-based services and long-term care services for most of the 385,000 Kansans in Medicaid/CHIP. The state in-turn pays the MCOs for the care. The majority of adults that are eligible for Medicaid are included in KanCare.
Implications of Medicaid Expansion
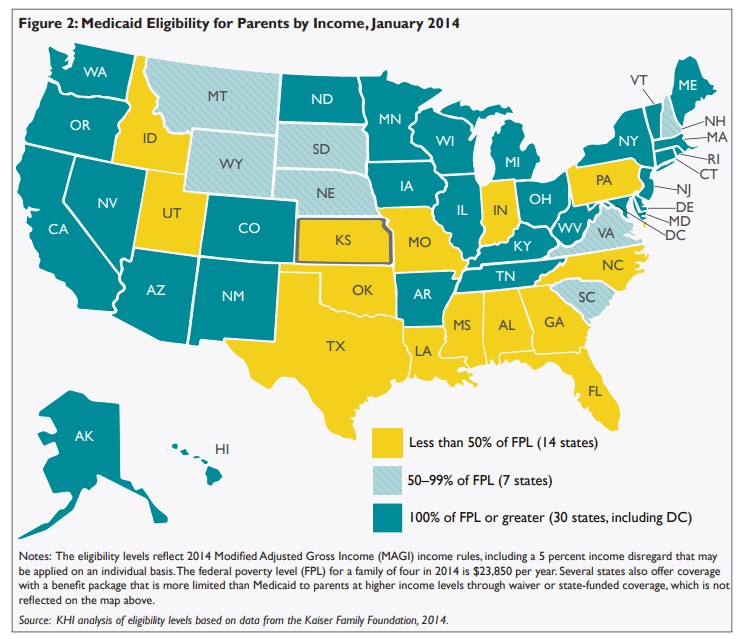
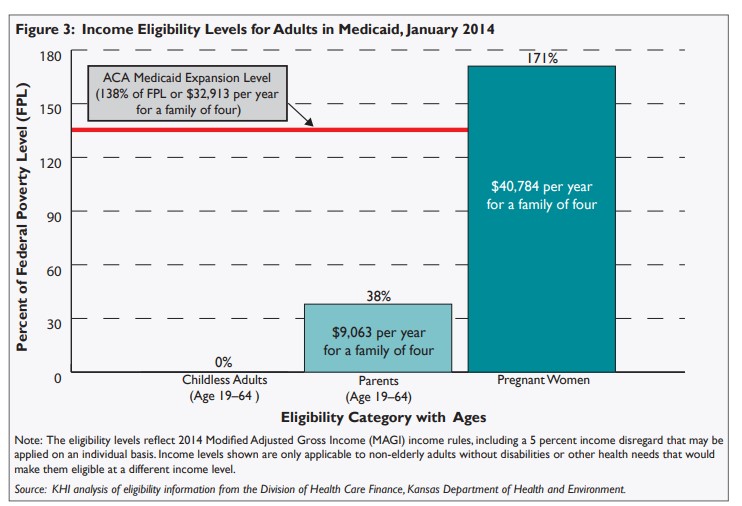
The ACA expands Medicaid eligibility to all adults with annual incomes up to 138 percent of FPL. However, the June 2012 U.S. Supreme Court decision that upheld the ACA made Medicaid expansion essentially optional for states. As a result, governors and state legislators across the country are evaluating how the expansion could affect the size and cost of their Medicaid programs. As of April 2014, Kansas officials had not expanded the program to cover adults whose individual or family income is under 138 percent of FPL.
The U.S. Census Bureau estimates that 324,000 Kansans age 19 to 64 have income below 138 percent of FPL. Of those, about 131,000 are uninsured. If Kansas decides to expand Medicaid, KDHE estimates that about 151,000 Kansans who were not previously eligible would sign up for Medicaid.
KDHE estimates that Medicaid expansion would increase spending by a total of $9.2 billion between 2014 and 2023. The federal government pays the majority of the cost for the newly eligible adults that would gain coverage through Medicaid expansion. The state’s cost of Medicaid expansion would total $1.1 billion over the same period. This includes the cost of newly eligible Kansans as well as additional adults and children that would enter Medicaid as a result of the “woodwork” effect.
The woodwork effect occurs as children and adults who are currently eligible for, but not enrolled in Medicaid, choose to enroll. This increased enrollment could be due to the requirement for all individuals to have health insurance coverage, or a spillover from efforts to sign people up through the federal insurance marketplace created by the ACA. Either of these could expand the size of the Medicaid program. The state estimates that an additional 41,500 people will enroll in Medicaid through the woodwork effect, and the majority of these will be children.
If Kansas expands Medicaid, the newly eligible Kansans added to Medicaid would shift the makeup of the adult population in the Medicaid program. Medicaid expansion would allow parents to be eligible at an income level four times the current level. Medicaid expansion also would make health coverage available to childless adults, a group that is not eligible for coverage now unless they are over age 65 or have a disability.
Conclusion
There is a common misconception that all Kansans who are extremely poor qualify for Medicaid. In reality, only a few categories of non-disabled adults under the age of 65 qualify. These categories include primarily pregnant women, very poor parents and guardians, and a few others who have very specific health care needs. Policymakers face a decision about expanding Medicaid coverage to more low-income adults or maintaining current Medicaid eligibility levels.