Factors That Might Affect Enrollment and Costs
The insert included with this report illustrates some of the major differences among the various Medicaid expansion proposals that may be considered by the Legislature. A more detailed version is available online, and will be updated regularly.
SB 252 combines elements from other proposals described in this brief as well as a bill pre-filed by Senate Minority Leader Anthony Hensley in December. SB 252 would expand Medicaid to adults age 19-64 up to 138 percent FPL and includes monthly premiums “up to” $25 for those with income above 100 percent FPL. It also includes a hospital surcharge of up to $35 million, designed to fully cover state net costs associated with adult enrollment.
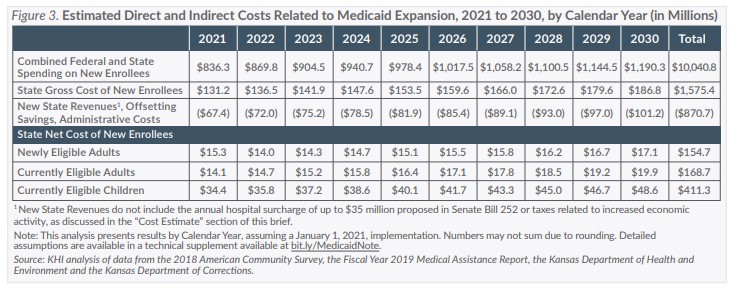
In association with the requirement for the state to submit a proposal for federal approval to create a reinsurance program for the individual health insurance marketplace, SB 252 also directs the state to request federal approval for adults with income between 100 and 138 percent FPL to be transitioned from Medicaid to ACA marketplace coverage by Jan. 1, 2022. The Centers for Medicare & Medicaid Services has not approved that authority in other states, but if the Kansas option were to be approved, it is estimated to reduce projected new enrollment by 34,504 adults and reduce net cost by $10.1 million in 2022.
Other provisions that have been debated in Kansas include work requirements. None of the current expansion proposals include work requirements, and while some, including SB 252, have work assessments and referrals, there are no associated financial or enrollment penalties for enrollees. The potential impact on enrollment and costs of such program elements are not included in this estimate, but the state likely would incur additional administrative costs administering the program.
The House-passed bill, as amended, included premiums of $25 to be collected from newly eligible enrollees, regardless of income. It also included a three-month lockout period for nonpayment and a permanent enrollment ban after a second episode of nonpayment. CMS has not approved cost-sharing above a nominal level for enrollees with income under 100 percent FPL, and generally has not approved disenrollment for that group. It also has not approved a permanent enrollment ban. If the proposal were to be adopted and approved, it is projected that about 37,000 potential newly eligible adult enrollees would either never enroll or at some point fail to make payments after initial enrollment and be disenrolled.
While 90 percent of the value of premiums collected would effectively reduce the federal share, the remaining 10 percent, or $1.6 million per year, would accrue to the state. However, the costs of administering the premium would be shared equally between the state and the federal government, and the premiums also would reduce some of the offsetting savings associated with expansion, as premiums would not apply to current eligibility groups. As a result of the administrative cost and lost savings, implementing premiums as proposed in the House bill could increase the net cost of expansion to the state by up to $4.5 million in the first year.
By allowing the state to implement a sliding scale premium structure, applying it only to those with income above 100 percent FPL, allowing hardship exemptions and not including a lockout period, the premium structure in SB 252 would have a lower impact on enrollment and costs. However, it is still likely that the state cost of administering the premiums would exceed the funds that would accrue to the state.
Finally, outreach efforts will influence enrollment and cost. Most states that have expanded Medicaid have experienced incremental enrollment in Year 1, suggesting the potential for lower enrollment and overall cost in 2021. However, lower initial enrollment could lead to higher per capita costs, whether for the state or for managed care organizations, as those with greater medical needs would be more likely to enroll. While this estimate does not model incremental enrollment in Year 1, its potential effects could be considered by policymakers as they consider outreach and communication about expansion.
Access additional publications in the Documents & Downloads section.