Health Impacts
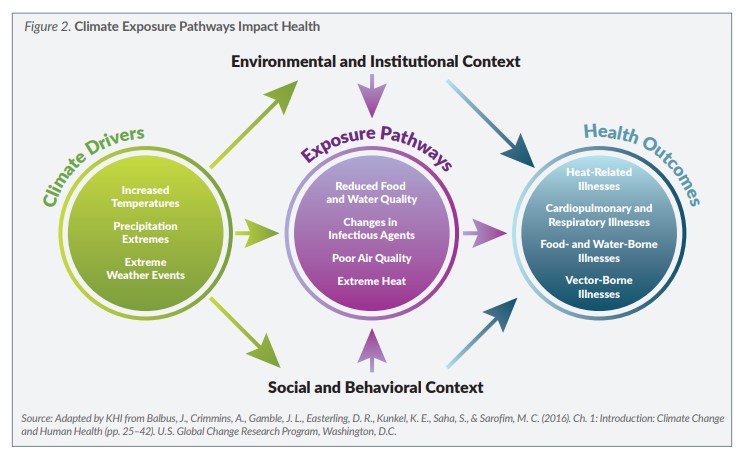
A conceptual model (Figure 2, page 3) shows the exposure pathways through which changes in climate can impact human health. Climate drivers create exposure pathways that interact with other factors (e.g., social, behavioral, environmental, institutional) to affect health outcomes. The extent to which climate change impacts the burden of disease depends on local climate factors, individual and population vulnerabilities, environmental exposure and capacity to manage risk. For example, rates of cardiovascular diseases, respiratory diseases and other chronic conditions are likely to increase, particularly among vulnerable populations, under projected climate change scenarios. Also, people with dementias, mental illness and disabilities are more vulnerable during extreme weather events such as heat waves, floods and tornadoes.
In Kansas, extreme heat and air quality are the pathways most likely to have the largest impact on health.
Temperatures
Exposure to higher temperatures and extreme heat can increase body temperatures to unsafe levels, stressing vital organs – such as the heart, lungs, kidneys and brain – and increase the risk of heat stroke and other heat-related injuries or illnesses. Hospitalizations for respiratory and cardiovascular conditions have been observed to increase during extreme heat days, particularly for chronic airway obstruction, asthma, ischemic heart disease and cardiac dysrhythmias. Hospitalizations and deaths due to heat-related causes vary substantially from year to year in Kansas. Between 2000 and 2014, heat-related illness hospitalizations ranged from a low in 57 in 2004 to a high of 180 in 2011. The heat-related death toll between 2000 and 2012 was also highest in 2011, at 37. Fewer than 5 deaths occurred in 2002, 2004 and 2010. The true burden is likely much higher, as these numbers reflect only those deaths in which exposure to excess heat was listed explicitly on the death certificate.
The elderly, very young, people with certain medical conditions, urban residents and laborers working in extreme heat are at greater risk of dying from heat stress. Studies report increases in cardiovascular and respiratory mortality, higher kidney failure rates and more hospital admissions among older adults during heat waves.
Prolonged exposure to extreme heat increases perspiration and decreases urination, which stresses the kidneys, leading to kidney stones and chronic damage over time. The 50-percent higher prevalence of kidney stones in the southeastern part of the country versus the northwest has led the former to being called the “kidney stone-belt.” As temperatures rise across the country the stone-belt is projected to spread northward, encompassing Kansas by 2050.
Warmer temperatures increase the length of the season for insect vectors of transmissible diseases. Fewer hard winter freezes will contribute to more mosquitoes and ticks, increasing the risk of insect-borne diseases such as West Nile virus and Lyme disease. Since 1970, the risk of disease transmission by mosquitoes has increased by 13 days per year in the northern part of Kansas, and 18 days in the southern part. Mosquito-borne disease cases were 35 percent higher in 2016 than in 2004. Kansas has experienced a dramatic increase in tick-borne diseases cases, which were 20 times more common in 2016 (251) than in 2004 (12).
Air Quality
Ozone and PM less than 10 microns (PM10) can be inhaled into the lungs, causing airway muscles to constrict, trapping air in the lung alveoli. Particles smaller than 2.5 microns (PM2.5) can penetrate deeper into the lungs and enter the circulatory system. Impacts range from minor upper respiratory irritation, wheezing and shortness of breath, to acute respiratory infections and chronic conditions such as chronic obstructive pulmonary disease (COPD), lung cancer, aggravation of heart and lung conditions, and asthma attacks. Short- and long-term exposures to PM2.5 are linked with reduced life expectancy.
Warmer temperatures lead to a longer plant growing season and greater pollen production. The mid-section of America has seen the pollen season increase by 10-18 days since 1995. A longer period for pollen production will expand the allergy season and worsen asthma symptoms. Allergies and asthma also will worsen in response to higher levels of CO2 and pollutants in the air. Higher CO2 concentrations increase the amount of ragweed pollen, the main contributor to hay fever. Air pollutants (particulate matter, CO, NO2, SOX) have been shown to increase the effects of aeroallergens (fungal spores, tree and weed pollens) in people with asthma.
Can Future Health Impacts be Estimated for Kansas?
Researchers have attempted to quantify the future impact of climate change on health at the regional, national and global levels. Can these studies be used to predict what will happen in Kansas, specifically, regarding increases in deaths, illnesses and injuries? The greatest sources of uncertainty in predicting health impacts are the climate modeling system and emission mitigation scenario used. The base epidemiological study and data, and population projection used, also are important. As a result, predictions vary markedly. For example, studies on ozone-related mortality suggest that by 2030, the number of additional deaths in the U.S. could range from 12 to 2,500.
Given the inherent variability in the methods and scenarios used by researchers, precise quantitative projections from the present literature are difficult, particularly for smaller geographic areas like states. However, some aspects of the potential health effects of climate change, such as temperature and air quality on mortality, have been widely studied. While research to quantify other medical and social impacts has been more limited, epidemiological studies and models suggest that the prevalence of cardiovascular, respiratory and certain other chronic diseases will increase in response to higher temperatures and declining air quality.
It is imperative that state and local governmental officials and other stakeholders in communities across Kansas develop strategies to mitigate the potential negative health effects as they develop climate preparedness and resiliency plans.
For more information about this subject, visit info@khi.org for the list of reference materials used in this analysis.
Access additional publications in the Documents & Downloads section.