Introduction
Medicaid program, called KanCare, will rely on private companies known as managed care organizations (MCOs) to coordinate the physical and behavioral health care, community-based services and long-term care services for the more than 380,000 Kansans in Medicaid.
This year Kansas will spend about $3.2 billion on Medicaid. With KanCare, the state hopes to save about $1 billion over five years.
Kansas has awarded contracts to three MCOs, which each will build a statewide network of providers for the full range of Medicaid services. Starting in 2013, each MCO will be assigned a proportional share of the Kansans in Medicaid, representative of different regions, age groups and populations, including people with disabilities, the elderly and low-income children.
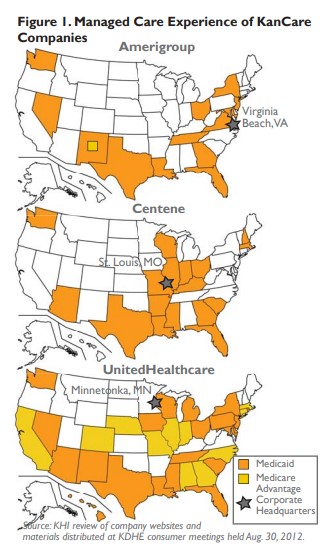
Figure 1 provides some details about the companies that were successful in winning a state contract to coordinate Medicaid services. Each map shows the MCO corporate headquarters, and states where the MCO has a contract for Medicaid and/or Medicare Advantage services.